Memorial Hermann The Woodlands Medical Center
- Open 24 Hours
General Information
Rooted in the Woodlands for nearly 40 years, Memorial Hermann The Woodlands Medical Center has provided family- and patient-centered, trusted care to the many communities of Montgomery County, north Harris County and beyond. We regularly invest in campus expansions to tailor our advanced, personalized services for you and your family. Here, you can realize why Memorial Hermann The Woodlands is your medical center.
Our welcoming campus, located at 9250 Pinecroft Drive, consists of a 457-bed main hospital with three patient bed towers and four professional office buildings. A team of nearly 1,200 affiliated physicians representing nearly 90 medical specialties, further enhanced by over 3,150 employees.
We are a designated Level II trauma center and were the first, and for more than a decade the only hospital in Montgomery County granted Magnet® status – an international distinction for nursing excellence and quality care by the American Nurses Credentialing Center. Learn more about nursing at Memorial Hermann The Woodlands »
This Is Your Medical Center in The Woodlands
We think the latest advances in health care should be close to home, not miles away – we are YOUR medical center.
Memorial Hermann The Woodlands brings together the ultimate in health care technology, expertise and healing for families in south Montgomery County, north Harris County and surrounding communities.
Specialties
- Breast Care Center
- Cancer Services
- Children's Services
- Diabetes Management
- Digestive Health
- Ear, Nose, and Throat
- Emergency Services
- Heart & Vascular Care
- Imaging Services
- Joint Center
- Mischer Neuroscience Center
- Neuroscience Services
- Orthopedics & Sports Medicine
- Physical and Occupational Therapy
- Robotic-Assisted Surgery
- Rockets Sports Medicine Institute
- Spine Care
- Surgical Services
- TIRR Memorial Hermann Inpatient Rehabilitation
- TIRR Memorial Hermann Outpatient Rehabilitation
- Trauma Services
- Weight Loss Surgery
- Women's Memorial Hermann
- Wound Care
For the Comfort of Our Patients & Visitors
Our all private room hospital includes enhancements like room service and sleeper sofas for family caregivers, where visitors and patients can access free wireless Internet through the MH_GUEST network to communicate with family and friends. Additionally, discover new campus features including a larger, relocated gift shop and expanded cafeteria and dining areas. Enjoy our Café-on-the-Go with Starbucks barista services, Market Coffee in the South Tower also with Starbucks barista services and snacks, a chapel, the Healing Garden, and Wolf Park with its own dedicated playground and seating area. Explore and be inspired by the hospital's many pieces of artwork including local and Texas photography, abstract paintings and multimedia sculptures.
In an effort to address community health and shape a healing environment, Memorial Hermann The Woodlands is a tobacco-free campus. No one may use tobacco inside or on the grounds outside the hospital or its surrounding medical plazas or parking garages.
Restricted tobacco products at and around our facilities, include cigarettes, e-cigarettes (vaping), pipes, and chewing tobacco. If you are a patient in need of tobacco, please reach out to your physician about a nicotine patch or ask us about resources for quitting tobacco use.
Expansion & Renovation
Memorial Hermann The Woodlands’ new South Tower is now open and its $250+ million expansion project moves into its final phase of renovation. Read About Our Expansion
Proud to be Part of One of the Region’s Largest Health Systems
Memorial Hermann The Woodlands is part of Memorial Hermann Health System, with more than a 110-year history of caring for the greater Houston area. Memorial Hermann is a 17*-hospital system, which includes Memorial Hermann-Texas Medical Center and Children’s Memorial Hermann Hospital; both are Level I Trauma Centers in Houston’s Texas Medical Center.
*Memorial Hermann Health System owns and operates 14 hospitals and has joint ventures with three other hospital facilities, including Memorial Hermann Surgical Hospital First Colony, Memorial Hermann Surgical Hospital Kingwood and Memorial Hermann Rehabilitation Hospital-Katy.
2019 Community Health Needs Assessment
As a part of providing Community Benefit to enhance the health and well-being of the residents of the Greater Houston area, Memorial Hermann Memorial City Medical Center is required by the Patient Protection and Affordable Care Act to identify the community’s health needs and strengths by conducting a Community Health Needs Assessment (CHNA) to prioritize health issues, to provide a foundation for the development of a community health improvement plan, and to assist community organizations in their program planning. Learn More.
Parking Information
All parking on the campus of Memorial Hermann The Woodlands is free of charge. Surface parking is available in lots located off Pinecroft Drive, the I-45 southbound feeder road and Medical Plaza Drive. Visitors may chose Parking Garage 2 (in front of MP2) for covered parking, using Levels A-D. There is a pedestrian sky bridge connecting the garage to the new South Tower from Level D.
Free valet parking is available on weekdays during peak visiting hours in front of our main hospital entrance at the new South Tower off Medical Plaza Drive and also currently outside of Medical Plazas 2,3 and 4 (until construction of Garage 4 is completed). After hours, valet keys may be picked up from the Security office on the first floor of the South Tower.
Golf carts round the parking lots to pick up visitors and patients, bringing them to hospital entrances and to medical plaza office buildings. There is a smaller parking garage (Garage 1) in front of Medical Plaza 1 (MP1), but this is for patients using services in that building. Garage 3 is for employee parking only and a staff badge is required.
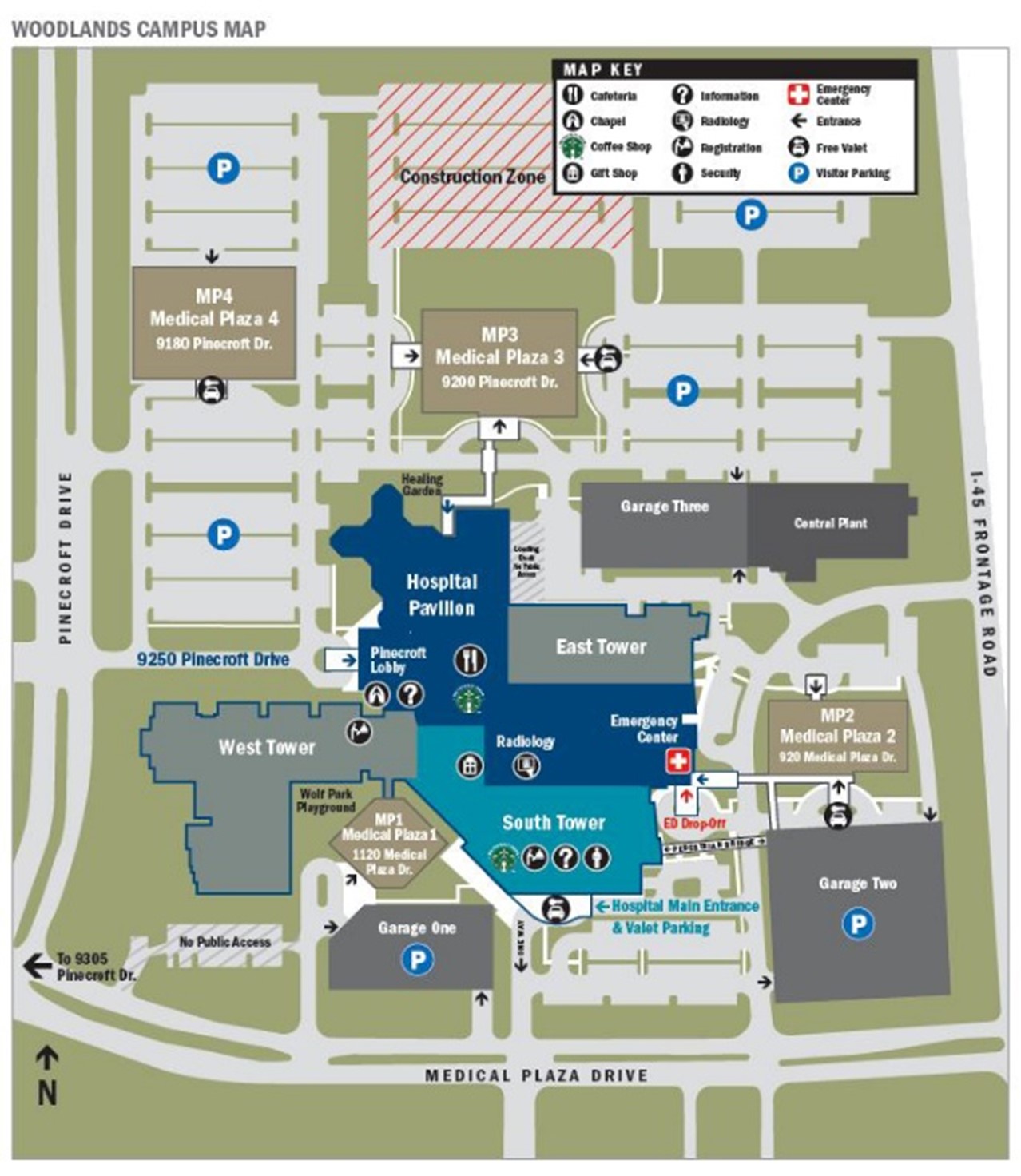
Campus Map
Click the map below to see and print a larger campus map.