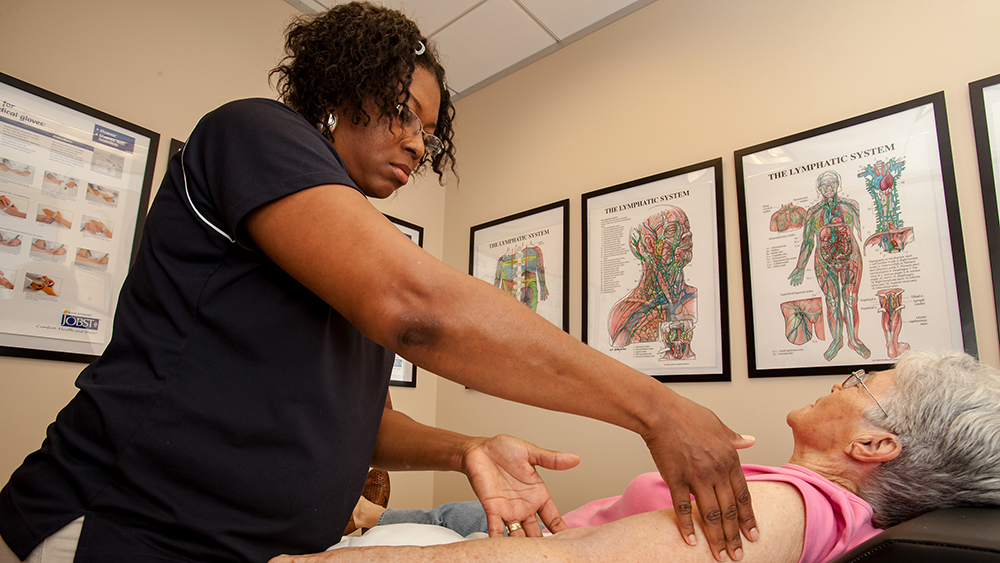
At Memorial Hermann, our team of affiliated occupational therapists, physical therapists, speech and language pathologists, social workers and neuropsychologists is specially trained to help you manage your lymphedema and provide treatments for other issues that may stem from the condition.
At Memorial Hermann, our team of affiliated occupational therapists, physical therapists, speech and language pathologists, social workers and neuropsychologists is specially trained to help you manage your lymphedema and provide treatments for other issues that may stem from the condition.
Focused on providing you with the best possible outcome, we use evidence-based treatment plans and tailor our program to your individual needs and medical history.
What is Lymphedema?
Lymphedema is a disease of the lymphatic system that causes persistent swelling of certain body parts, particularly the legs, arms, face or genitalia.
The lymphatic system plays a critical role in your body’s immune system by shuttling white blood cells through a network of lymph vessels to fight infection. In several places throughout your body, there are small collections of tissue called lymph nodes that help the lymphatic system filter out harmful substances and fight infection. If this system is damaged through infection, surgical removal of lymph nodes or other means, it can cause the buildup of lymph fluid in the fatty tissues just beneath your skin.
What Are the Common Causes of Lymphedema?
There are two main types of lymphedema:
- Primary Lymphedema is a hereditary condition without an obvious cause, though it is believed to be a result of improper development of the lymphatic system.
- Secondary Lymphedema has several potential causes, including:
- Surgery to remove cancerous tumors and affected lymph nodes
- Radiation therapy
- Chemotherapy
- Infection or other trauma to the lymphatic system
Cases of lymphedema stemming from cancer treatments are on the decline. According to the Lymphatic Education and Research Network, treatments such as breast cancer surgery once carried a 50% risk of lymphedema development. Now, thanks to advances in medical technology and increased awareness of this condition, the risk has dropped to only 15%-25%. For patients who don’t have to undergo additional adjuvant radiation therapy to lower the chance of their cancer returning, the lymphedema risk is as low as 6%.
Signs and Symptoms
Contact your doctor or nurse when symptoms first appear, as early diagnosis and treatment prevent complications. Some signs and symptoms of lymphedema may include:
- A full or heavy feeling
- Texture changes in the skin
- Aching or discomfort
- Less movement or flexibility in nearby joints such as your shoulder, hand and wrist
- Trouble fitting into jewelry and / or clothes in one area such as the sleeve of your jacket, a pant leg or sock
- Tingling
- Numbness
Precautions
In order to decrease the risk of developing or the worsening of existing lymphedema symptoms, the following precautions should be taken:
- Avoid extreme hot and cold temperatures
- Avoid hot baths and showers
- Avoid saunas and hot tubs
- Avoid insect bites
- Avoid skin punctures, needle punctures, cuts and acupuncture to the swollen limb
- Avoid pet scratches
- Avoid blood pressure cuffs on the affected limb
- Avoid wearing tight clothes, rings or watches on the affected limb
- Avoid deep massage or swedish massage
Lymphedema Treatment
While lymphedema cannot be cured, it can be effectively treated. If you’re interested in finding relief through lymphedema therapy, you’ll first need a referral from your primary care physician. We will then schedule a one-hour evaluation session with one of our trained staff members. Based on this evaluation, we will create a custom lymphedema management program that follows the principles of Complete Decongestive Therapy.
Your custom program will include:
- Manual lymphatic drainage (MLD), which uses light massage to help lymphatic fluid flow from the swollen area
- Topical skin and nail care to eliminate bacterial and fungal growth and resist infection
- Compression bandaging to prevent lymph fluid from re-entering affected extremities
- Therapeutic exercises to help muscles pump excess lymphatic fluid away from the affected area
- Diet and nutrition counseling to help you maintain a healthy weight
Each session will run from one to one-and-a-half hours in length, four to five days a week, for up to six weeks (or until maximum volume reduction is achieved). When therapy is complete, your specialist will instruct you and your family on proper self-maintenance techniques so you can practice lymphedema management at home.
Phase One: Intense Treatment Phase
An evaluation consists of a one-hour session with subsequent lymphedema treatment sessions of 1-1.5 hours in duration. You will receive treatment four to five days per week for an average of 4-6 weeks or until maximum volume reduction is achieved. Complete Decongestive Therapy incorporates:
Manual Lymphatic Drainage
This light touch massage is used to help open lymph channels and allow lymphatic fluid to flow from the swollen area. Effective in promoting wound healing in areas of edema, or swelling, this also helps break fibrotic tissue resulting from chronic edema.
Manual lymphatic drainage (MLD) facilitates reabsorption of large protein molecules found in lymph fluid and increases the frequency of lymph vessel contraction. MLD consists of specific light, rhythmic pressure along lymphatic pathways that empties and releases obstructive lymph vessels, stimulating the movement of lymph fluid along the vessel pathway.
Hygiene and Topical Skin Care
Lymphedema patients are at increased risk of infection, making education in skin care techniques imperative. We teach meticulous skin and nail care and the use of pH-balanced skin lotions that eliminate bacterial and fungal growth.
Bandaging and Compression
Bandaging follows each manual lymphatic system drainage session. Bandages are minimally elastic and prevent lymph fluid from re-entering the affected arm or leg. When lymphedema is reduced to an acceptable level, patients are custom-fitted with an elastic compression garment.
Contraindications for Manual Lymphatic Drainage:
- Congestive heart failure
- Local or acute infection with fever or undiagnosed swelling
- Deep vein thrombosis
- Presence of a malignant tumor
Therapeutic Exercise Instruction
Therapeutic exercise is one of the lymphedema drainage methods that involves movement of the affected extremity, vital to the reduction of edema. There are simple lymphatic drainage exercises that allow muscle contractions to assist in pumping excess fluid out of the body via veins and lymphatic vessels. Our therapists work with patients to exercises their limbs while using compression bandages. Exercise enhances the compression function of bandages.
Diet
To promote optimal edema control, it is important for patients to maintain a healthy weight that is in proportion to their body height and frame. We also recommend that patients limit their intake of salt and monosodium glutamate (MSG). Our therapists provide further nutrition information over the course of the therapy.
Phase Two: Self-Maintenance Phase
Once maximum volume reduction is achieved, you will be measured for compression garments which you will wear during the day. Additionally, you will use bandages at night or alternative nightwear compression. You will continue to perform exercises, skin/nail care, self-manual lymphatic drainage as well as attend follow-up visits with your certified lymphedema therapist as needed.
Find Relief with Lymphedema Therapy at Memorial Hermann
Don’t suffer with lymphedema pain in silence. Memorial Hermann has several lymphedema clinics throughout the Greater Houston area, and we can help you find relief and manage your symptoms.
Use our online cheduling tool or fill out the form on this page to schedule your initial lymphedema evaluation today.
Find Relief with Lymphedema Therapy at Memorial Hermann. Don’t suffer with lymphedema pain in silence. Memorial Hermann has several lymphedema clinics throughout the Greater Houston area, and we can help you find relief and manage your symptoms. Use our online scheduling tool or fill out the form on this page to schedule your initial lymphedema evaluation for physical therapy treatment today.