
Pectus excavatum, estimated to occur in 1 of every 300 to 400 births, disproportionately affects males, and tends to accelerate during the teenage years; in some cases it’s identified at birth, but not always. While its effects on the appearance of those diagnosed can be a serious concern— problems with self-esteem and body image are common— the condition also may cause physiological issues. “The chest is normally round or oval-shaped, but in these kids, it kind of sinks down,” explains Dr. KuoJen Tsao, chief of general and thoracic pediatric surgery at McGovern Medical School at UTHealth and chief of pediatric surgery and the pediatric pectus program at Children’s Memorial Hermann Hospital. “They may or may not be able to expand their chests, which allows them to breathe.”
Soon after Palomino was diagnosed, the family found Dr. Tsao. The procedure to correct pectus excavatum, the surgeon explained, involves inserting a metal bar into the chest between the sternum and the heart in order to push out the sunken breast bone. Using small surgical cameras, the bars are placed through small incisions in each side of the chest to ensure proper placement, and to avoid injury to the heart and lungs.
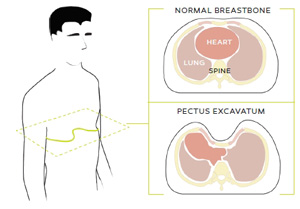
Did you know? Pectus excavatum, a genetic condition that causes the breastbone to sink into the chest, is estimated to occur in 1 of every 300-400 births and mostly affects males.
But no matter when the surgery takes place, it can be tough on the patient. “It can be quite uncomfortable initially,” says Dr. Tsao, though a combination of numbing the nerve endings and pain medication helps substantially. There’s also the risk of infection and bleeding, and proximity to the heart is always a concern. But the procedure, Dr. Tsao affirms, is fairly safe. “I remember the doctor saying, ‘We’re near the heart. We’re near the lungs during this procedure,’” Palomino’s mother, Heidi Daley, recalls. She wasn’t certain she wanted her son to have it done. “A lot of it was driven by him,” she says. “I was pretty hesitant about it. But he was dead set on it, and we had a great, great surgeon in Dr. Tsao. That helped a lot.”
Dr. Tsao successfully performed the procedure on Palomino when he was 16. And while the healing process was slow and challenging, the teenager was thrilled with the results. “It was a difficult process,” says Palomino, now 19 and a biomedical engineering student at the University of Utah. “It was about a month’s recovery, and it was really painful.” It took him nearly five months to feel completely normal again. “But, if I had the choice,” he says, “I would do it again.” Palomino didn’t realize his condition had been affecting him physically until he began to heal. “After the surgery, I definitely noticed a difference,” he says. “It was a lot easier to breathe when I would do cardio.”

The change in how a child feels about him or herself, he adds, can be life-altering. “A big part of this, which is really hard to document, is how important it is for people to have great self-esteem,” he says. “My goal is to make their chest a non-issue.” This year, the bar that was inserted in Palomino’s chest was removed through an outpatient surgery that caused little or no pain, and today the student, a workout enthusiast, has only a few small scars to show for the ordeal. His happiness with his overall appearance is apparent, especially to his mom. “The appearance thing was insignificant to me, but it was important to him,” she says. “I think he definitely feels happy about it now—over the top, in fact. We get tired of hearing about it.”