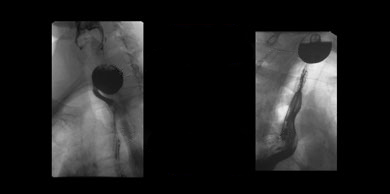
Zenker's diverticulum is a pouch at the back of the throat, above the cricopharyngeal muscle (where the pharynx and esophagus join). This muscle can malfunction (fail to relax or open easily), resulting in an out-pouching of the posterior wall of the pharynx, just above the esophagus. Food and saliva will accumulate in the pouch over time and the pouch will grow in size.
What Are the Causes of Zenker’s Diverticulum?
Malfunctioning of the cricopharyngeal muscle with aging seems to be the main cause. Some neurologic diseases, such as a stroke, may result in malfunctioning of the cricopharyngeal muscle.
What Are the Symptoms of Zenker’s Diverticulum?
A small Zenker’s diverticulum can be asymptomatic (exhibit no symptoms). When a diverticulum increases in size, the following symptoms may appear:
- Dysphagia (difficulty swallowing)
- Regurgitation (return of undigested food back into the mouth)
- Sense of a lump in the neck
- Halitosis (smelly breath) due to stagnant food in the pouch
- Cough, especially at night
- Hoarseness (voice change)
- Involuntary gurgling noises when swallowing
- Pneumonia due to aspiration of food in the windpipe
How Is Zenker’s Diverticulum Diagnosed?
A videoesophagram is the most effective way to diagnose a Zenker's diverticulum. The barium used in the procedure fills the pouch, making it visible in the upper part of the esophagus, as shown in the picture below.
Upper endoscopy allows assessing the inside of the diverticulum and the size of its opening. The procedure needs to be done very carefully and by expert hands to prevent esophageal perforation.
Contact Us
If you have questions or are looking for more information, please complete the form below and we will contact you.