Memorial Hermann Heart & Vascular Institute at Southeast Hospital
General Information
Memorial Hermann Southeast Hospital is part of the Memorial Hermann Health System, one of the world’s largest providers of cardiovascular care, treating more than 200,000 patients a year. Our team of affiliated cardiologists, cardiothoracic and vascular surgeons, clinicians, researchers and educators are developing and perfecting innovative techniques that continue to put Memorial Hermann at the forefront of advancing heart health in Houston.
Awards and Recognition
American Heart Association Mission: Lifeline® STEMI Silver Receiving Plus Quality Achievement Award
The American Heart Association has awarded it the Mission: Lifeline® STEMI Silver Receiving Plus Quality Achievement Award to Memorial Hermann Southeast Hospital. The Receiving Awards are given to hospitals that implement specific quality improvement measures outlined by the American Heart Association for the treatment of patients who suffer severe heart attacks.
Chest Pain Joint Commission Certified and PCI Facility
Memorial Hermann Southeast Hospital’s designation as a certified Chest Pain Center recognizes the affiliated physicians and hospital staff for meeting the Society of Chest Pain Centers’ stringent criteria for rapid response.
Memorial Hermann Southeast Hospital is designated as a Percutaneous Coronary Intervention (PCI) hospital. This means all types of chest pain patients, from low-risk disorders to acute myocardial infarction, can be assessed and treated in our cardiac catheterization labs. At 90 minutes or less, the STEMI team’s fast times to PCI meet the “gold” standard for door-to-balloon times.
Services
Preventive Care
It all starts with preventive care. Specially-trained physicians affiliated with Memorial Hermann Southeast Hospital can assess your risk for heart and vascular disease, prescribe lifestyle modifications and/or medication, perform noninvasive and invasive diagnostic tests, such as cardiac catheterization, and coordinate with other specialists for more complex care.
Other preventive programs include:
- Wellness and weight management programs
- Nutrition consultations
Heart Imaging and Diagnostics
Successful treatment and survival of a heart attack requires immediate medical attention. The affiliated heart specialists utilize advanced technology to assist in providing fast, accurate diagnosis and treatment of coronary artery disease, close to home.
- Tilt-table test
- Echocardiography
- Transthoracic
- Transesophageal echocardiography
- Stress echo
- EKG
- Holter monitor
- Exercise/chemical stress testing
- Nuclear cardiology
- Peripheral vascular ultrasound
- Vein mapping
- Arterial Doppler ankle-brachial index
Chest pain patients are screened for heart attack symptoms upon arrival to our Emergency Center and, if necessary, are transferred to our 24/7 ST-Elevated Myocardial Infarction (STEMI) STEMI cardiac catheterization lab.
Accredited Chest Pain Center and PCI Facility
Memorial Hermann Southeast Hospital’s designation as an accredited Chest Pain Center recognizes the affiliated physicians and hospital staff for meeting the Society of Chest Pain Centers’ stringent criteria for rapid response.
Memorial Hermann Southeast Hospital is designated as a Percutaneous Coronary Intervention (PCI) hospital.
This means all types of chest pain patients, from low-risk disorders to acute myocardial infarction, can be assessed and treated in our cardiac catheterization labs. At 90 minutes or less, the STEMI team’s fast times to PCI meet the “gold” standard for door-to-balloon times.
Vascular and Endovascular Services
Vascular and Endovascular Capabilities include:
- Aortic surgery
- Abdominal aortic aneurysm (AAA) repair
- Aortic root reconstruction
- Thoracoabdominal aneurysm (TAA) repair
- Endovascular surgery
- Aortic aneurysm repair
- Thoracic aortic aneurysms (TEVAR procedure)
- Carotid artery stenting
- PAD
- Peripheral vascular surgery
- Carotid endarterectomy
- Thoracic outlet syndrome (TOS)
- Limb salvage and critical limb eschemia
- Surgery/ablation for varicose veins
- Dialysis access surgery
Thoracic Surgery
Memorial Hermann Southeast Hospital offers an array of thoracic services, from diagnostic procedures to innovative minimally invasive surgery that are shown to improve outcomes for rare and common forms of chest and lung disease.
Thoracic capabilities include:
- Minimally invasive lung surgery
- Video-assisted Thorascopic surgery (VATS)
- VATS lobectomy
- VATS thymectomy
- Minimally invasive esophagectomy (MIE)
Cardiac Rehabilitation
Whether you have had a heart attack, bypass surgery, angioplasty, heart transplant or valve replacement, or have angina, congestive heart failure or any other cardiac-related illness, you may benefit from the cardiac rehabilitation program at Memorial Hermann Southeast Hospital. Our goal is to help people with heart disease participate actively and confidently in their own recovery so they can return, as much as possible, to the life they enjoyed before heart disease.
The cardiac rehabilitation program is a three-phase, multidimensional, medically supervised program designed to help patients recover as quickly as possible from heart disease. With a comprehensive focus on exercise, education and lifestyle change, the program is designed to improve overall physical and mental functioning. Patients who participate in a cardiac rehabilitation program following heart surgery or a diagnosis of heart disease tend to have better outcomes in managing their condition.
*Physician referral is required for outpatient cardiac rehabilitation.
Memorial Hermann Southeast Hospital's Cardiovascular Surgery Program Anniversary
Learn more about the 5th anniversary of the cardiovascular surgery program at Memorial Hermann Southeast Hospital.
Parking Information
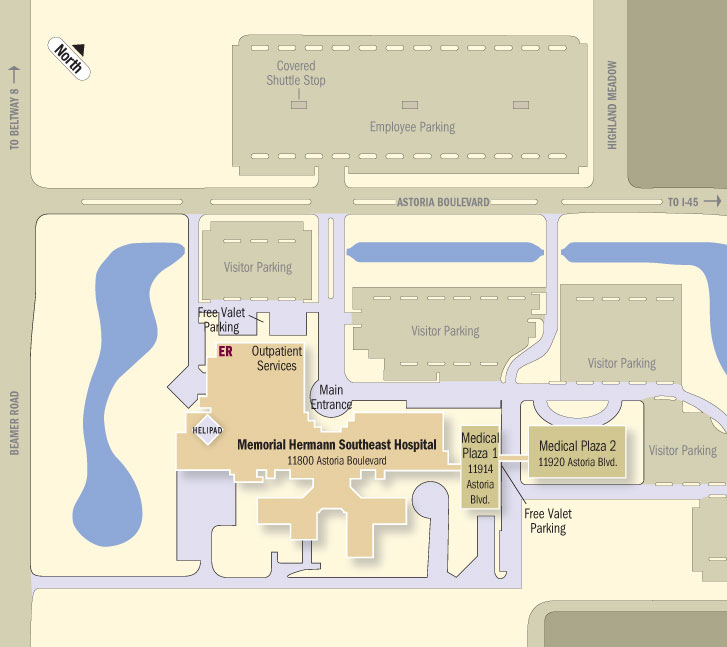
Complimentary valet parking is available outside Outpatient Services building, at the Medical Plaza II building entrance and between Medical Plaza I and II. Free parking is available in the visitor lot in front of the main hospital entrance, and handicapped parking is clearly identified. Please do not park along the hospital’s front curb. This is a fire zone and should only be used for patient drop-off and pickup.
Contact Us
Please fill out the fields below and we will contact you, or call (713) 222-2273 for more information.