By Charlotte Huff
Photos by Michael Starghill Jr. for Stat
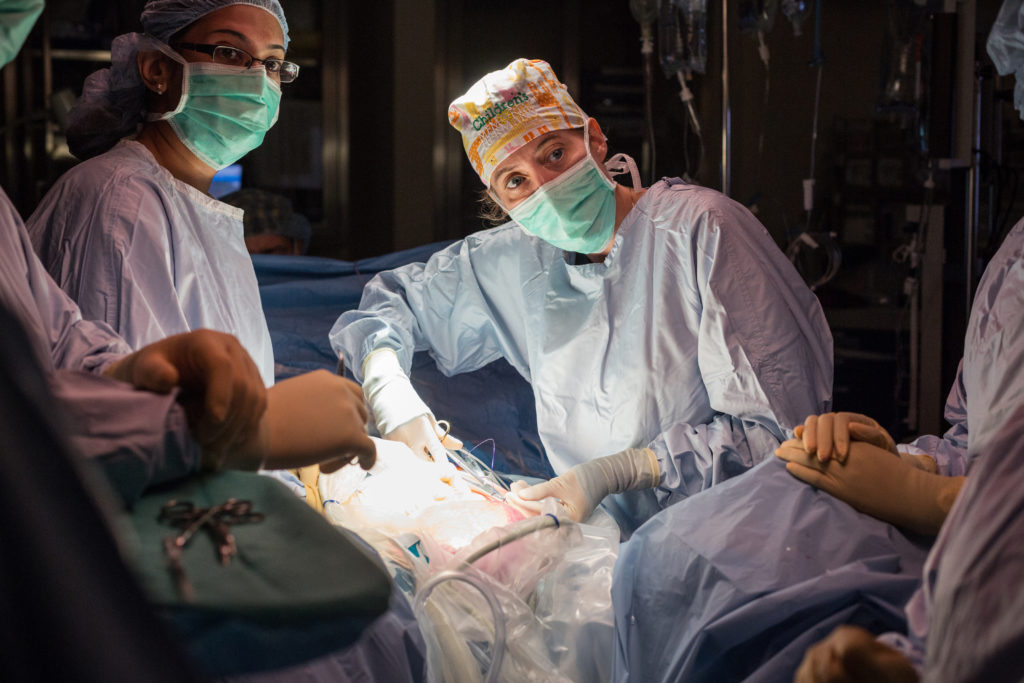
For many years, Dr. Mary Austin could count on one hand the people who knew.
There was her close friend through middle school, who helped her pee by pushing on her lower abdomen. Years later, during her surgical training at Vanderbilt University, she confided in a mentor. Her husband knew, of course.
But until now, she hadn’t told even some of her close colleagues — or her patients.
Sometimes these patients are pregnant women, wrestling with a daunting decision: Whether to consent to a delicate surgery on their babies, in utero, to try to close a hole around the fetus’ spinal cord.
The birth defect is called spina bifida. Untreated, it can cause a range of disabilities, from incontinence to learning difficulties to an inability to walk. But the surgery carries some risks, too; it can send the mothers into premature labor, months before their due dates — and there’s no guarantee it will prevent physical disabilities in the baby.
Austin, a pediatric surgeon, helps counsel couples through that agonizing decision. She walks them through the potential risks and benefits. She describes each step in the hours-long surgery, from slicing open the uterus to closing the gap around the spinal cord with tiny stitches through developing fetal tissue so fragile, it’s almost “like tissue paper,” she said, vulnerable to tearing.
What she doesn’t tell them: She herself has spina bifida.
Taking a risk for an unborn son
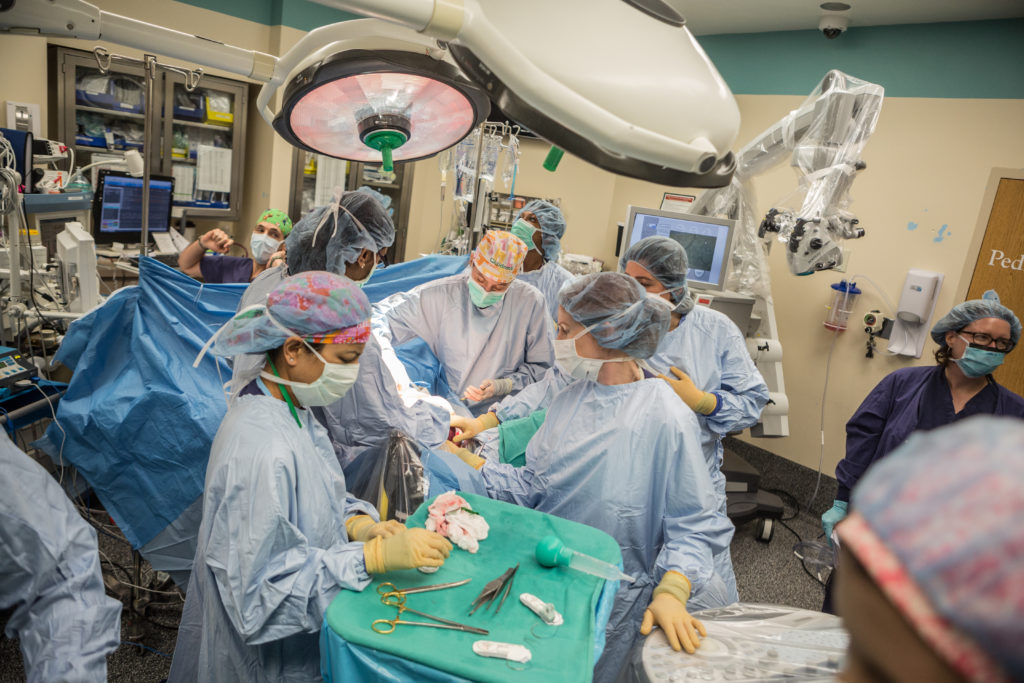
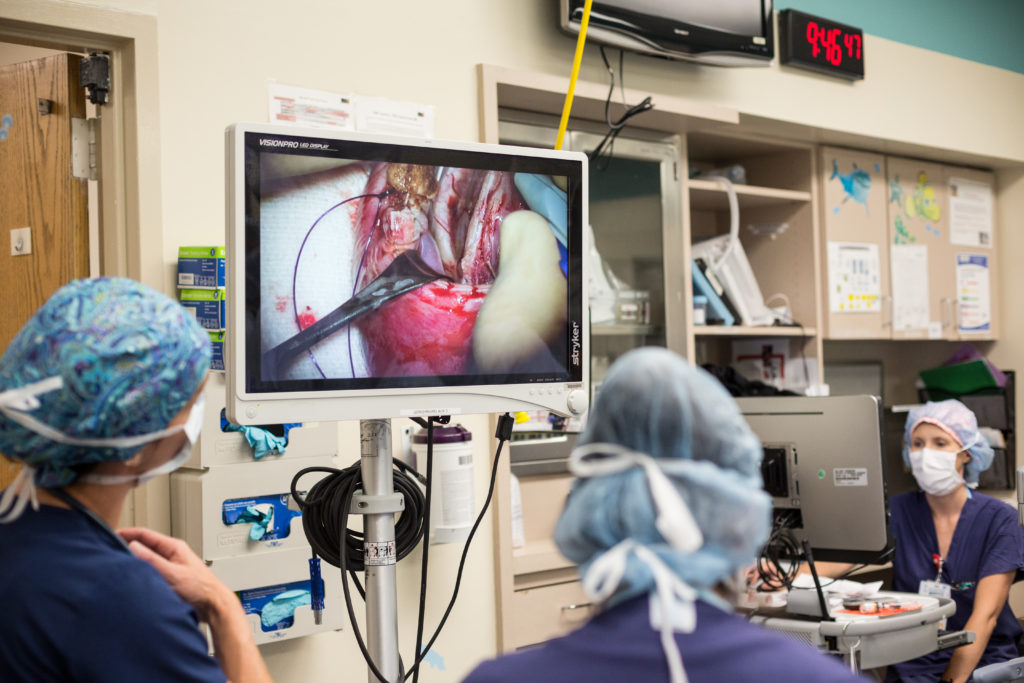
Dressed in blue scrubs and colorful surgical caps, Austin and several other surgeons bent over their patient, Cassi Young. The operating room at Children’s Memorial Hermann Hospital, crowded with clinicians, was hushed.
A surgeon made the first incision, exposing Young’s watermelon-sized uterus. The team then methodically worked their way inside, slicing through tissue and muscle to reach her fetus. The slightly burnt smell of cauterized tissue permeated the air. A sonographer stood at the end of the table, monitoring the baby’s heart rate and providing regular updates to the surgical team.
Young and her husband, David, had named the baby Luke David. Their first child, he’d been diagnosed nearly two months earlier, back home in Oklahoma City. The news was a shock, as neither of them knew anything about spina bifida.
A doctor in Oklahoma City first raised the possibility that the birth defect could be repaired in utero. So the Youngs traveled to Houston for several days of testing and counseling with specialists at a fetal center that’s affiliated with Children’s Memorial Hermann Hospital and the University of Texas Health Science Center at Houston.
The surgery’s goal: to stall any further damage. The doctors noted that Luke met several criteria, including that his little legs were moving in utero, visible on ultrasound. That made him a good candidate for surgery, they said.
The couple decided to go for it. The operation would give their son “the best chance for quality of life,” Cassi Young, 30, said the day before the surgery. Her eyes held steady as she spoke, yet she was clearly anxious about what was to come.
During her pregnancy, she had avoided even acetaminophen to protect her baby. “Now I’m going to let them cut me open,” Young said.
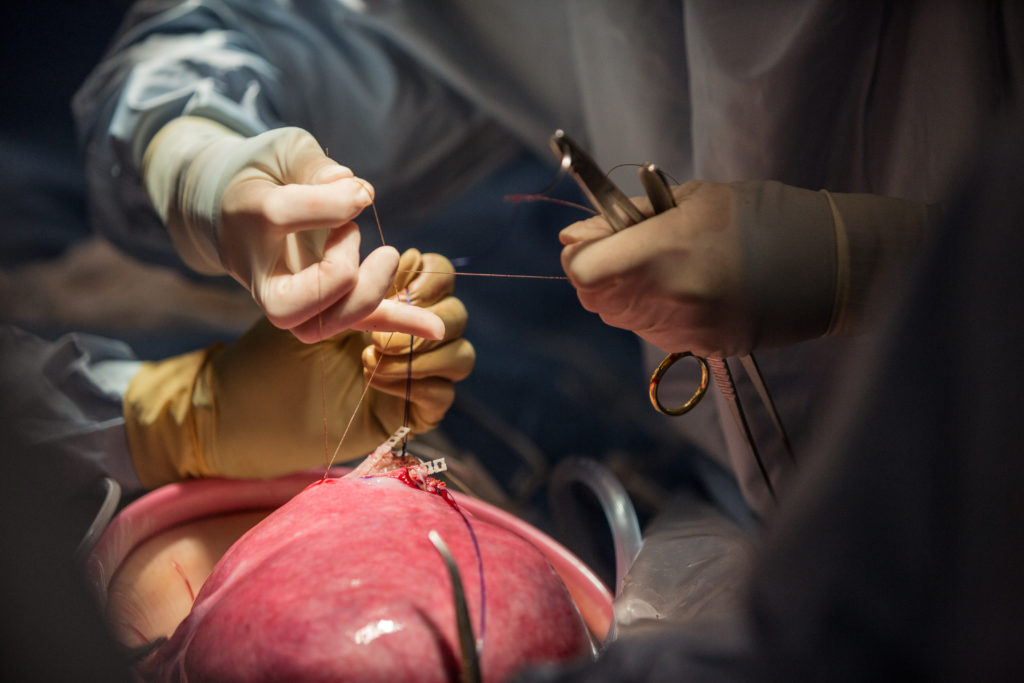
Inside the operating room on that May morning, the surgeons moved deftly. Soon, they had reached Luke, just 1 pound, 9 ounces at 26 weeks gestation. They saw the lesion: a small area around the spinal cord, less than 2 inches long.
That’s what they would need to close.
‘I wanted to be a normal kid’
About 1,500 U.S. babies are born each year with the type of spina bifida that Luke and Austin have, called myelomeningocele. Its severity depends upon a number of factors, among them how high up on the spinal cord the opening is located and which nerves are exposed. Austin, whose lesion was repaired shortly after birth, has a relatively limited case.
Still, doctors at first were dubious that Austin would ever be able to walk. Her mother, Judy Austin, a physical therapist, didn’t buy the dire predictions: “I thought, ‘These people don’t know what they are talking about.’”
As it turned out, the doctors were flat out wrong. From childhood, Austin didn’t need any help to walk. And soon she was running, endless miles, right up until a recent knee operation temporarily slowed her pace. Now 43, Austin regularly bikes to work, unfazed by the swampy Houston summers. In fact, she first got to know her husband, Dr. Andras Heczey, when they both competed in the Solvang Century, a 100-mile bike race.
But Austin also has lived from birth with what’s called a neurogenic bladder and bowel, which means that the nerves required for proper functioning have been damaged. And growing up in the rural town of Horse Cave, Ky. — where her parents operated two tourist attractions, a cave and a park with kangaroos and other exotic animals — she had little opportunity to consult with specialists. (“I literally grew up in a zoo and in a cave,” Austin explained, with a laugh.)

Until Austin learned how to catheterize herself in her early teens, when her parents took her to a spina bifida clinic a few hours away, she relied on her parents and her close friend to help release her urine. She was so fearful her bladder might betray her with an accident, she didn’t pursue cross country or track in high school, though she loved to run.
She doesn’t remember opening up to anyone else about her spina bifida in high school or in college, even roommates. “It embarrassed me,” she said. “I wanted to be a normal kid, a normal young adult. I guess I got so used to hiding it — it was just natural. It wasn’t a lot of work to do that.”
Despite her best efforts, though, she’s coped with countless urinary tract infections through the years, and sometimes, kidney infections. She swallowed stool softeners regularly while growing up, with mixed success. Several times, her parents raced to the emergency room to relieve painful backups. Learning how to self-administer enemas in medical school “changed my life,” she said.
The whole time, her mother said, “Mary always has been — even with me throughout her life — very closed about her problem. She just absolutely did not want it to interfere in any way with her goals.”
She had set one of those goals by kindergarten: She wanted to become a doctor. Her vision for her medical future sharpened after she had an operation in her early teens to make sure that her spinal cord wasn’t affected by scarring from the initial surgery.
It embarrassed me. I wanted to be a normal kid.
Austin still remembers the pediatric neurosurgeon involved who did the operation. As she puts it, he was “a piece of work.”
“While I’m sure he was fine as a technician, I don’t think the man ever spoke two words to me.”
She resolved to do better when she became a doctor.
A mentor probes — and gets the truth
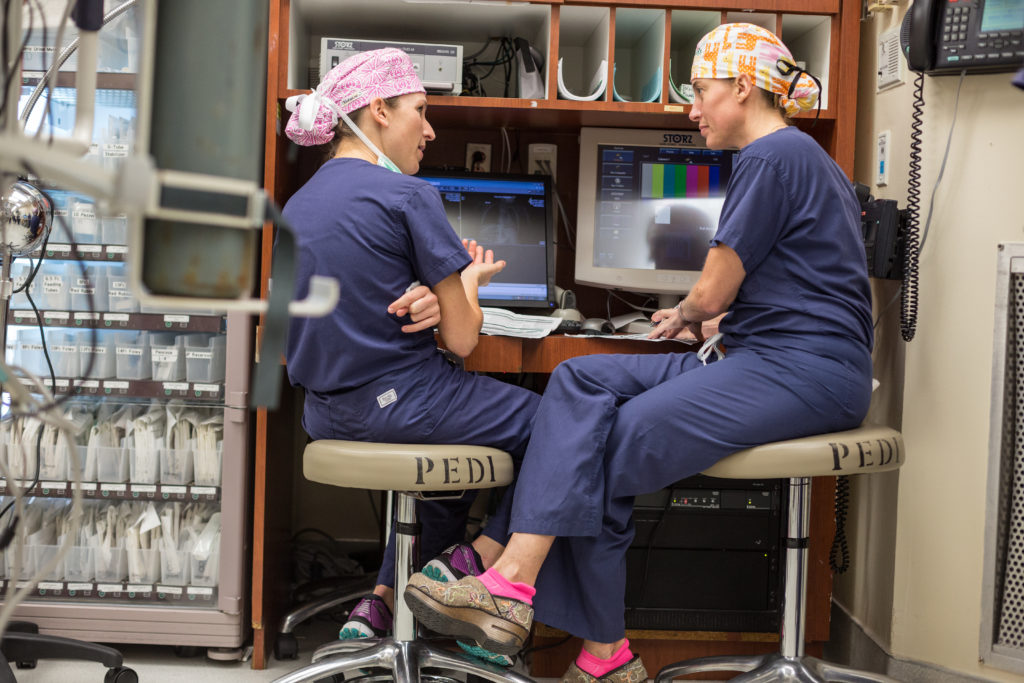
The day before operating on Young, Austin had a jam-packed schedule, which kicked off at 7 a.m. with an emergency abdominal surgery on a struggling premature baby. By 2:30 p.m., when she paused for a bowl of tomato soup, she had completed or supervised six surgeries, including two appendectomies and a gallbladder surgery on a 17-year-old new mom.
“Dr. Austin, how do you feel about this stitch?” a senior resident she was supervising in the operating room called out at one point.
In between, she checked on a steady stream of patients in the neonatal intensive care unit or on the hospital floors. She popped in on a young girl whose esophagus was being repaired over a series of procedures, and a 14-year-old boy with a bit of a mustache who would soon be rolled into the operating room. “When you wake up, you’ll be minus an appendix you don’t need,” she said, leaning over his bed with a smile.
She indulged in a few yawns along the way. (She’d been on call the prior night and her pager had gone off some 10 to 15 times.) But she never slowed down. “You’ve just got to keep moving,” she said, her flower-embroidered clogs striding across the floors of Children’s Memorial Hermann.
Austin learned the nonstop pace during her surgical residency, which required 100-plus hour weeks. She was dogged, prepared, and had “moxie,” said Dr. James O’Neill, a surgical mentor at Vanderbilt University Medical Center.
One day, though, he remembered her looking pale and unwell: “I knew her, and something wasn’t right.”
So he asked. Austin admitted first to a urinary tract infection — and then to their frequency. O’Neill, worried, pressed further. Finally, she disclosed the underlying cause: her spina bifida.
It was a rare moment of vulnerability in the ultra-competitive world of surgical training, where physician residents are loath to show any weakness, O’Neill said. “She’s such a hard worker — I think she didn’t want to get into a position where she might have to give up surgery.”
It was O’Neill, who oversaw surgical services at Vanderbilt for many years, who insisted that Austin get a full checkup by a specialist in spina bifida.
Those specialists mostly deal with babies and children. So Austin, then in her early 20s, found herself in a pediatric neurosurgeon’s office. When she checked in, she was asked: “What’s your child’s name?”
The neurosurgeon gave her a clean bill of health. As it turned out, he was one of the pioneers of the in-utero spina bifida surgery that Austin helps to perform today.
Austin didn’t consider having kids herself as she worked her way through a decade of residency training after medical school. Then she wondered if she had waited too long; she was 36 when she married Heczey. Her periods had always been irregular.
But she was soon pregnant — in fact, she’d wrapped up a half Iron Man triathlon before she even realized it.
Spina bifida, though, made staying pregnant more difficult. Austin’s neurogenic bladder boosted her risk of urinary tract and kidney infections. Her first child, Bella, was born six weeks early, after various infections landed Austin in the hospital five times, finally triggering premature labor. Her second pregnancy went more smoothly and her younger daughter, Lily, was born full term in 2012.
These days, she’s raising 4-year-old and 6-year-old girls, part of a two-physician couple, with all of the logistics that entails. The evening before Young’s operation, she had swung by the grocery store to replenish food and the woefully scant dog food supply and buy flowers for teacher appreciation day.
When she’s asked the proverbial “How do you it all?” her response is quick, with a wry smile: “Not very well.”
Guiding parents through a wrenching decision
At the time that Austin was born, the only option for babies with spina bifida was to repair the gap around the spinal cord immediately after delivery. But starting more than 15 years ago, a few medical centers began to operate before birth. And a multi-hospital randomized study, published in 2011, showed that earlier intervention could help.
In-utero surgery was not a cure. 40% of babies who had it still had to have a shunt implanted in their brain later to drain spinal fluid accumulating in the skull — a fairly common complication of spina bifida.
Still, that was a big improvement: Among babies who weren’t treated until after birth, 82% needed a shunt.
The babies who got in-utero surgery also were twice as likely to be able to walk without braces or other help — 42% achieved that milestone, versus 21% in the other group. The American College of Obstetricians and Gynecologists has since recommended that eligible women should be educated about the option.
When Austin and other physicians at the fetal center sit down with couples, they share the national study data and the results they’ve seen at their fetal center. Based on the center’s first 32 cases analyzed, the odds that the baby will get a shunt after delivery are roughly similar to the national average. The possibility of the baby being born very premature, before 30 weeks, is somewhat lower at the center — 6% versus 13% in the national data.
A woman must consider other factors, too. The surgical incision could rupture if she gets pregnant again, complicating her ability to have additional children. She must commit to bed rest until delivery, something that work and family circumstances might not permit.
When she talks with couples, Austin does not mention that she, too, has spina bifida. She wants them to focus on the research data and their personal circumstances rather than making assumptions about how their baby will fare, based on her energetic persona and hard-charging career as a pediatric surgeon.
“I don’t want them to see me as this outcome that they expect their unborn child to have,” Austin said, “and then make a decision based on that.”
A hole, a patch, a moment of relief
The surgery to repair the hole in Luke’s spine was the 48th such operation the center had done. The surgical team exchanged only a few quiet words as they worked, faces tight with concentration.
The room was filled nearly to overflowing with more than a dozen clinicians, including doctors, nurses and technicians, as well as an anesthesiologist focused on Young and another for Luke. In an adjacent room, not much larger than a walk-in closet, a neonatal transport team was waiting, in case the surgery ended in a premature delivery.
One of the nurses kept David Young updated by text. She sent a picture of Luke’s spinal cord opening, visible on the video monitors surrounding the operating room table. And then later, another photo, once it had been closed.
Austin’s gaze was intent on her sutures, her long, dark blond hair hidden beneath a surgical cap with colorful giraffes. Her primary role during the nearly three-hour surgery was to open the uterus and expose Luke in preparation for the repair by the pediatric neurosurgeon. She’d then assist with closing the uterus.
Before that repair began, Luke was given several medications to help guard against pain, keep his heart rate normal, and prevent him from moving during the surgery. The team drained the amniotic fluid surrounding him, setting it aside to return later.
Luke’s lesion was too large to close with stitches alone; if surgeons tried to pull the skin edges together, they risked tearing it. So they applied a patch, made of cow tissue.
Afterward, Austin — still in her scrubs and giraffe cap — went to update David Young, who was anxiously waiting along with Cassi’s mother and sister. Luke had done well; his heart rate had been good, Austin told them. But it wouldn’t be until well after his birth that they would know whether the repair had helped.
Cassi Young was in the hospital recovering five days later when her contractions started. They couldn’t be stopped. She was three months from her due date, and Luke was still perilously small.
But he was coming.
An obstetrician was called for an emergency C-section. Austin, who was being updated along with the rest of the surgical team, had just flown in from a medical meeting. She changed quickly and went to the hospital, in case she was needed to assist.
She literally held my hand [going] to the OR to deliver him. I probably was squeezing her hand to death.
Luke David Young was born May 7, a tiny bundle with dark hair, weighing just 2 pounds, 1 ounce. He stretched slightly more than 13 inches long.
As of mid-June, Luke was a bit heftier, 3 pounds, 5 ounces. His lungs were still developing, so he needed a ventilator to breathe. But the skin on his back had grown over the patch so his parents — until then only able to touch their son through an opening in his incubator — were finally able to hold him. It was amazing, his mom said, to feel him lying skin to skin against her chest.
And he’s moving his legs, his feet, his ankles, his toes. “He is a wiggle worm,” she said.
Austin, who stops by to check on Luke every few days, said he still faces the challenges of any premature baby. But it’s a good sign that he’s moving his legs and that he’s peeing and pooping on his own. Whether he’ll have any bladder difficulties once he starts potty training, or whether he struggles to walk, only time can tell.
‘It would have given us more hope’

Austin knows that it might appear her spina bifida has never slowed her down. But she vividly recalls the freakout she had as a teenager, when she realized that she’d have to learn how to catheterize herself.
And she remembers the isolation — the feeling that she was the only one her age with such challenges.
It’s that memory that has spurred her to speak out more in recent years, at first to colleagues and then to a reporter. She wants teens with birth defects to know they’re not alone — and she wants parents to seek consultations with specialists, even if it seems as though their children are coping.
Shortly before this article was finalized, Austin shared her spina bifida diagnosis with Cassi and David Young.
“I’m pretty sure, my husband and I, our jaws just dropped to the ground,” Cassi Young said.
They understood why Austin hadn’t told them earlier — why she hadn’t wanted them to be thinking of her as they debated how best to help their unborn baby. They respected her decision.
But Cassi Young also said that Austin shouldn’t worry that future patients might look her up online and read about her lifelong struggles, and triumphs, with spina bifida.
“If she would have told us in that room, when we met with her, I think it would have given us hope,” she said. “Not so much that [her success] is going to happen to us. It would have just given us more hope.”
This story was originally published on Stat News.
Contact Us
To contact The Fetal Center at Children's Memorial Hermann Hospital, please fill out the form below.
If you are experiencing a medical emergency, call 911 or go to the nearest emergency room.
If you or someone you know needs support from the Suicide and Crisis Lifeline, call or text 988.
Located within the Texas Medical Center, The Fetal Center is affiliated with McGovern Medical School at UTHealth Houston, UT Physicians and Children’s Memorial Hermann Hospital.